|
2/7/2024 0 Comments Hemothorax lung sounds 
Distended neck veins are concerning for pneumothorax or pericardial tamponade but might be absent in the setting of hypovolemia. Inspect the chest wall for signs of contusion, abrasions, "seat belt sign," penetrating injury, paradoxical movement ("flail chest”), ecchymosis, deformities, crepitus, and point tenderness. Ĭlinical findings of hemothorax are broad and may overlap with pneumothorax these include respiratory distress, tachypnea, decreased or absent breath sounds, dullness to percussion, chest wall asymmetry, tracheal deviation, hypoxia, narrow pulse pressure, and hypotension. The mechanisms of action that were predictive of significant thoracic injury are motor vehicle accident greater than 35 mph, fall from more than 15 feet, pedestrian ejection of more than 10 feet, and trauma with depressed level of consciousness. Important history components include chest pain, dyspnea, mechanism of injury (fall, direction, and speed), drug/alcohol use, comorbidities, surgical history, and anticoagulation/antiplatelet therapies. Thorough and accurate gathering of history from the patient, witnesses, or prehospital providers helps determine those patients that are at low vs. These mechanisms result in tension hemothorax physiology and cause hemodynamic instability, cardiovascular collapse, and death. A large hemothorax can lead to an increase in hydrostatic pressure which exerts pressure in the vena cava and pulmonary parenchyma causing impairment in preload and increase pulmonary vascular resistance. Blood in the pleural space affects the functional vital capacity of the lung by creating alveolar hypoventilation, V/Q mismatch, and anatomic shunting. In the early response, acute hypovolemia leads to a decrease in preload, left ventricular dysfunction and a decrease in cardiac output. The severity of the pathophysiologic response depends on the location of the injury, the patient's functional reserve, the volume of blood, and the rate of accumulation in the hemithorax. Early physiologic response of a hemothorax has hemodynamic and respiratory components. 
Studies have shown that injury to intercostal vessels (e.g., internal mammary arteries and pulmonary vessels) lead to significant bleeding requiring invasive management. Each hemithorax can hold 40% of a patient's circulating blood volume. īleeding into the hemithorax may arise from diaphragmatic, mediastinal, pulmonary, pleural, chest wall and abdominal injuries. Lung ultrasound (US) in the evaluation for hemothorax has demonstrated accuracy, with higher sensitivity than chest radiography. Multiple studies have shown that chest ultrasonography is a valuable tool in the diagnostic approach of patients with blunt chest trauma. In addition to the traditional right and left upper quadrant views of the FAST, the operator can slide the probe cephalad to evaluate quickly for the presence of fluid above the diaphragm. Pulmonary windows have been included in the Extended-Focused Assessment with Sonography in Trauma (eFAST) protocol since the mid-2000s. It is usable at the bedside for triage and identification of life-threatening injuries. POCUS is rapid, reliable, repeatable, and most importantly, portable. Recent literature suggests point-of-care ultrasound (POCUS) can be useful as an adjunct to traditional imaging modalities. Chest radiography has been used traditionally as a screening tool to evaluate for immediate life-threatening injuries. Furthermore, smaller centers may not have CT scan readily available. Bleeding may arise from the chest wall, intercostal or internal mammary arteries, great vessels, mediastinum, myocardium, lung parenchyma, diaphragm, or abdomen.ĬT scan is the preferred method of evaluation for intrathoracic injuries however, it may not be feasible in the unstable trauma patient. 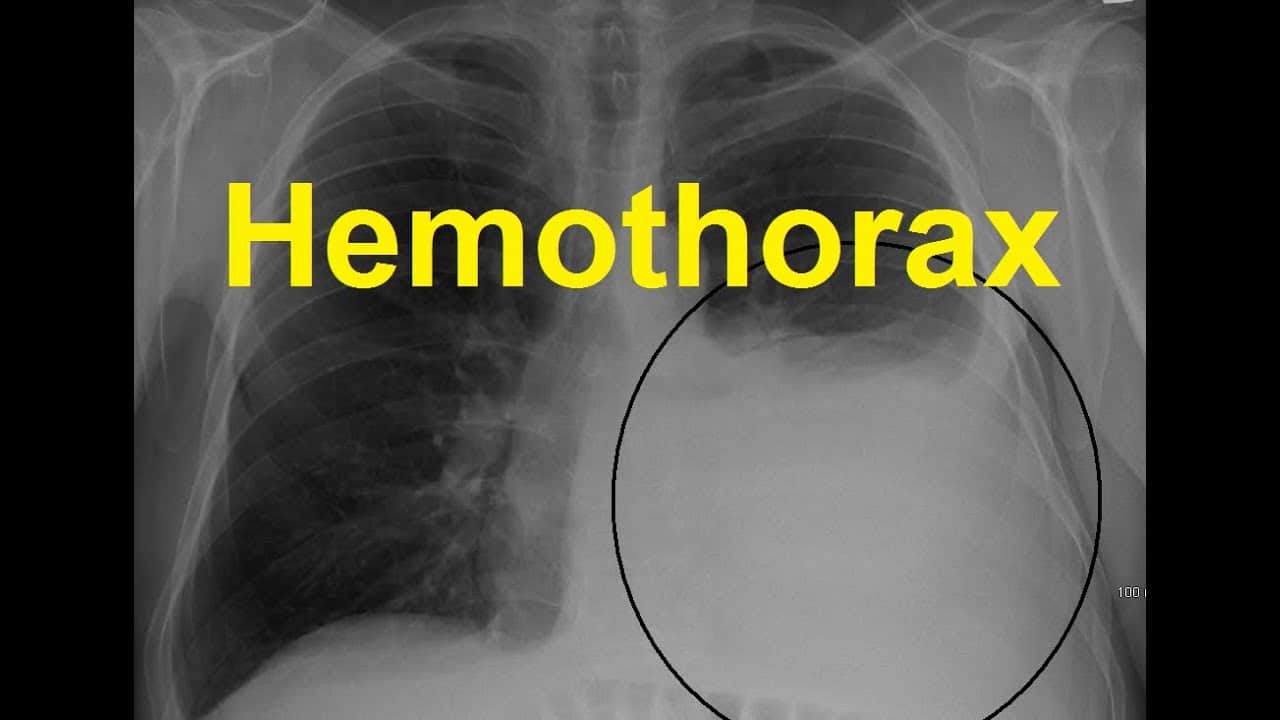
The most common mechanism of trauma is a blunt or penetrating injury to intrathoracic or extrathoracic structures that result in bleeding into the thorax. It is a collection of blood in the pleural space, a potential space between the visceral and parietal pleura. Hemothorax is a frequent consequence of traumatic thoracic injuries. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
